Introduction
The highest rate of infection is prevalent in Blacks and women. You may feel embarrassed, upset, or ashamed if diagnosed with genital herpes. However, it is a common infection that is painful but doesn’t cause life risks.
The culprit behind genital herpes is the Herpes simplex virus type 2 (HSV-2). Persons with HSV-1 are at risk of getting HSV-2 genital herpes.
Genital herpes causes painful genital sores. It spreads from skin-to-skin contact, and you may get it while kissing persons with open sores.
While there’s no cure for herpes, available genital herpes treatment options can lower the symptoms and prevent its spread.
What Is Genital Herpes? How Common Is Genital Herpes?
Genital herpes is an infection in the genitals. Genital herpes symptoms include blisters or lesions.
The sores appear near the vagina, buttocks, and anus in women, while men get them on the penis, buttocks, and scrotum.
The infected areas get a tingling or itchy sensation before the sores appear. Persons who contract the infection for the first time may have flu-like symptoms, including fever, body ache, and swollen glands. Sexually active teens and adults get the infection irrespective of gender and race.
Genital herpes is a common infection, and one out of six Americans suffers from it. Women, especially black women, are prone to HSV-2 infection that causes genital herpes.
Genital herpes causes include vaginal, oral, and anal sex with the infected persons. According to the CDC, 18.6 million Americans were infected with HSV-2 genital herpes, costing a burden of $91 million in 2018.
Often, patients with genital herpes have mild symptoms or remain asymptomatic. Infected persons may pass the infection to their partners unknowingly.
Who Might Get Genital Herpes? Where Does It Form?
Genital herpes is extremely contagious. Persons infected with HSV-1 and 2 can easily pass on the infection as they may not know they are shedding.
In many cases, genital herpes patients are asymptomatic. Women are especially vulnerable because, during unprotected sex, the delicate vaginal tissue can tear and easily infect the person. Women can get blisters on and around the labia, vulva, vagina, and buttocks.
Male genital herpes symptoms appear around the penis head, scrotum, buttocks, and thighs. Small red bumps may appear near the anus, and there could be a tingling or burning sensation during urination.
Types Of Herpes Viruses – How Many Do You Know Of?
HSV-1 and HSV-2 are the most known and discussed herpes viruses for their roles in spreading cold sores and genital herpes. However, six more herpes viruses frequently infect us, and scientists have classified them into alpha, beta, and gamma groups.
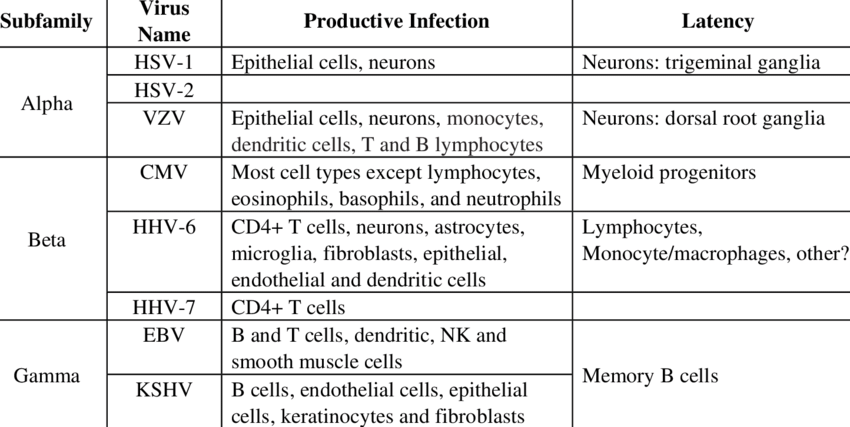
Image Credit: researchgate.net
- Alpha (α) Herpesviruses: HSV-1, HSV-2, and Varicella zoster virus (VZV) fall in this category. They have a very short reproductive cycle, can promptly destroy the host cells, and possess a speedy replication capacity in many host tissues.
HSV-1 is a common herpes virus and enters the body through cell membranes. The HSV-1 virus routinely infects persons aged between 14-70. HSV-1 targets the mouth and lips as well as genital areas. Lots of people infected with HSV-1 remain asymptomatic. The contagious virus spreads through kissing and oral sex.
HSV-2 is also a common alpha herpes virus, and the highly contagious virus spreads through skin-to-skin contact. Similar to HSV-1 patients, HSV-2 infected patients may remain asymptomatic. HSV-2 is found to be responsible for causing genital herpes. Unprotected sexual intercourse with infected partners spreads the HSV-2 virus. In limited cases, HSV-2 causes oral herpes after affecting the genitals.
There’s no definite curative genital herpes treatment for HSV-1 and HSV-2 viruses. Varicella-zoster virus is another type of alpha herpes virus that causes chickenpox and shingles. The extremely infective virus gives painful rash and itchy blisters. There have been approved vaccines for VZV in the US since 1995.
- Beta (β) Herpesviruses: Human cytomegalovirus (CMV), Human herpesvirus 6A and 6B, and Human herpesvirus 7 are included in this category. Beta Herpesviruses exhibit a long replication cycle and stay hidden inside the secretory glands, kidneys, and phagocytic cells. CMV is a common beta herpes virus with no cure, and different strains exist.
Signs and symptoms of CMV include swollen glands, sore throats, fever, joint pain, and fatigue. Symptoms generally disappear after 15 days. Recurring CMV infection may damage the lungs, eyes, and digestive system. CMV spreads through saliva, semen, blood, tears, breast milk, and urine. Persons with weak immunity may need medications.
HHV-6 and HHV-7 are two other extremely common beta herpes viruses responsible for fever, rash, flu-like symptoms, and diarrhea. HHV-6 and HHV-7 infections are observed during early childhood.
- Gamma (γ) Herpesviruses:Epstein-Barr virus (EBV) and Kaposi’s sarcoma-associated herpesvirus (KSHV) are the two Gamma herpes viruses that infect humans.
Epstein-Barr virus (EBV) is a common herpes virus that infects people worldwide. EBV spreads through saliva from kissing, shared utensils, toothbrushes, and children’s toys smeared with saliva.
HIV-infected untreated persons get affected by Kaposi’s sarcoma, a type of cancer characterized by tumors with blood vessels that appear below the skin’s surface and spread throughout the body. Kaposi sarcoma-associated herpesvirus is a carcinogenic virus that causes Kaposi’s sarcoma.
Genital Herpes Causes: HSV-1 And HSV-2 – Which One Causes Genital Herpes?
Genital herpes is a lifelong infection caused by HSV-1 and HSV-2 viruses.
According to traditional studies and research, HSV-2 is the culprit that causes STD genital herpes. However, recent research[1] doesn’t give HSV-1 a clean chit. A growing number of first-episode genital herpes have been linked to HSV-1. Both HSV-1 and HSV-2 viruses enter the body through broken skin or moist areas, including the vagina, mouth, and anus.
Let us now look at the most common genital herpes causes:
- Unprotected Sex With an Infected Partner-Unprotected vaginal, anal, and oral sex with an infected partner with oozing sores is the surefire way to get STD genital herpes. After making contact, the virus travels in the body through mucous membranes present at the opening of the nose, mouth, and genitals.
- Having Multiple Sex Partners-Having multiple sex partners increase the risk of sexually transmitted infections. High-risk sexual behavior is one of the reasons why female college students are prone to STDs, including genital herpes.
- Being Sexually Active at a Young Age-Today’s teens are susceptible to genital herpes. This study[2] mentions that the changing sexual practices are one of the reasons why young adults with HSV-1 infection are at the risk of getting genital herpes.
Recurrence is a crucial issue with genital herpes. After the initial outbreak, the virus stays in the nerve cells for the rest of life. Various internal and external triggers, as studies[3] show, may reactivate the virus from its dormant stage. Emotional distress, certain illnesses, sun exposure, surgeries, hormonal changes are responsible for waking up the virus.
Genital Herpes Symptoms

The contagious HSV-2 virus spreads through skin-to-skin contact. However, persons infected with herpes simplex type 2 may not have any symptoms, and some may get mild symptoms that they interpret as skin conditions, yeast infections, or vaginosis.
You may consider visiting a doctor if you notice any of the following genital herpes symptoms:
- Pain and itching in the genitalia, buttocks, and thighs
- Burning or tingling sensation while peeing
- Vaginal or penile discharge
- Painful sores or blisters around and near the genitals are symptoms of an infected person with the HSV-2 virus. The blisters are 1 to 3 mm in size. The fluid-filled lesions burst and ooze fluid before forming a crust. The blisters appear near the penis, scrotum, thighs, and buttocks in men. Women get them around the vagina, cervix, and external genitals
- The blisters burst to create ulcers that may cause pain during urination
- Scabs are formed after the ulcers heal
Genital herpes symptoms differ from person to person. Some may experience fever, joint ache, or swollen lymph nodes in the groin area, and fever during the initial phase. For some, lesions can be tender and painful, and some may not feel pain or discomfort.
Recurrence And Genital Herpes
Herpes infection is extremely contagious, and once the virus enters the body, it stays forever. Recurrent outbreaks are a common feature of STD genital herpes, and the first outbreak may span two to four weeks.
Do You Need To See A Doctor For Treating Genital Herpes?

Often, the first-episode genital herpes symptoms don’t appear. Persons infected with the HSV-2 may have mild symptoms, and some may confuse the symptoms with common skin conditions or yeast infections.
Though genital herpes is not fatal, complications can arise. Persons with HSV-2 symptoms should undergo tests if they notice lesions in genital areas, mouth, anus, and buttocks. Herpes blisters appear in clusters, and they burst and turn into sores that ooze or bleed.
If you notice symptoms, your healthcare provider may suggest viral culture tests or nucleic-acid amplification tests to detect if you have STD genital herpes.
On the other hand, if you think you have contracted the virus but haven’t noticed the classic symptoms associated with it, you may still consider an IgG test.
If you suspect you have genital herpes, consider making an appointment with the doctor fast! Timely medical attention may help you deal better with your infection and prevent future complications.
Additionally, medical guidance may help you avert the risks of meningitis, bladder issues, other STIs, skin and eye infections, and rectal inflammation.
Pregnancy And Genital Herpes
Herpes infection can be fatal for newborn babies. Pregnant women need to consult doctors if they have genital herpes. If women get genital herpes symptoms during the last trimester of pregnancy, there’s a 30-50% chance of passing the virus to the baby. It is, therefore, crucial to inform the doctor if there’s a sign of an outbreak.
Genital Herpes Treatment: What Options Do You Have?
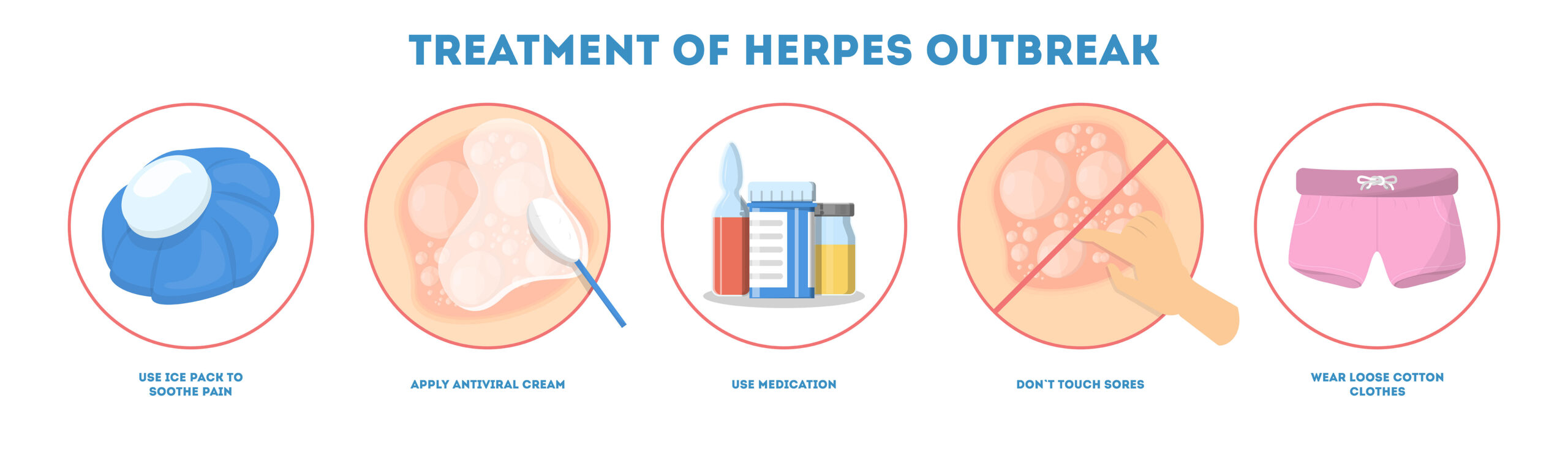
Genital herpes is a sexually transmitted infection, and unfortunately, the virus, once in, stays forever. Available genital herpes treatment prevents outbreak recurrences, alleviates the symptoms, and makes them disappear faster. Treatments also prevent the infection from spreading to another person.
A range of prescription medicines, self-care remedies, OTC products is available for genital herpes treatment. They include the following:
- Antiviral Drugs – Patients having the first episode of genital herpes outbreak are prescribed the FDA-approved antivirals available on the market. The FDA-approved antiviral medications are Acyclovir, Valacyclovir, and Famciclovir. These antiviral prescription medications accelerate healing and shorten an outbreak episode. Episodic therapy and suppressive therapy with antiviral drugs have been proven helpful in shortening outbreak periods. However, these medications may cause side effects. You should talk clearly to your doctor before taking any of these.
- Alternative Therapies – Alternative therapies are a way to deal with genital herpes symptoms. As this study[4] shows, Aloe vera gel has shown promising antiviral activity against HSV-2 replication. Essential oils such as tea tree oil, ginger essential oil, and chamomile essential oil have antiviral properties, and topical applications of these oils could be one of the options to get relief from the painful symptoms. Bee products such as honey and propolis may help alleviate painful lesions. This study[5] shows that honey treatment has helped with the complete remission of genital herpes.
How Can You Prevent Genital Herpes?
Preventing genital herpes requires awareness about the infection. As there’s no cure and as it is highly infective, you may consider taking the following tips:
- Opt for mutually monogamous relationships with a partner who is not infected.
- Know your partner’s sexual history before getting engaged in the act.
- Practice safe sex with latex condoms whenever you hit the sack.
- If your partner is infected, consult a doctor for regular anti-herpes medications.
- Don’t have sex during an outbreak.
- If your partner is infected, you may consider mutual masturbation instead of oral or vaginal sex.
Conclusion
What will you do if you are diagnosed with genital herpes? It may make you feel emotionally upset. As of late, there’s a social stigma around the condition. Having an STI may impact your social image, and it may even ruin your relationship with your partner.
But don’t lose perspective. Take time to adjust and seek immediate medical help. There’s no cure available yet, but antiviral medications may help your situation and keep it under control. These meds reduce the spread of infection.
And there are ways you can still enjoy togetherness with your partner. Educate yourself about the infection, join a support group, and go beyond genital-to-genital sex.
Mutual masturbation could be a way to satisfy your sexual needs, especially when your partner has an outbreak. Take safety measures as your healthcare consultant advises.








