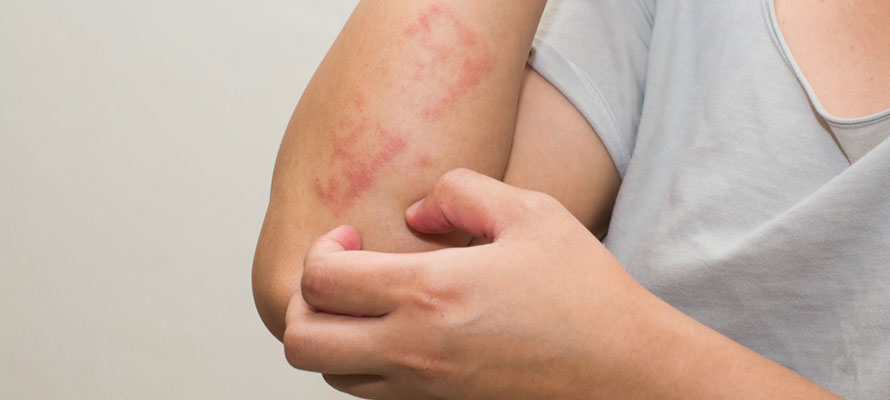
Eczema cannot be spread. You cannot “catch” it from another person. Researchers do know that individuals who get eczema do so as a result of a combination of genetic predispositions and environmental triggers, despite the fact that the actual origin of eczema is unknown.
Although adults can also have this skin disorder, children frequently do. In fact, 10% of people will experience eczema at some point in their lives, according to the National Eczema Association.
The most common cause of eczema, also known as “atopic dermatitis,” Atopic is the name for an allergy. People with eczema frequently have allergies or asthma in addition to itchy, red, or other types of skin conditions.
Atopic Dermatitis
Eczema, in its most prevalent form, is atopic dermatitis. It usually starts in childhood and gets less severe or disappears with age.
The atopic triad, as described by medical professionals, includes atopic dermatitis. “Triad” refers to three. Asthma, hay fever and allergies are the other two disorders in the trio. All three disorders are common among those who have atopic dermatitis.
Contact dermatitis
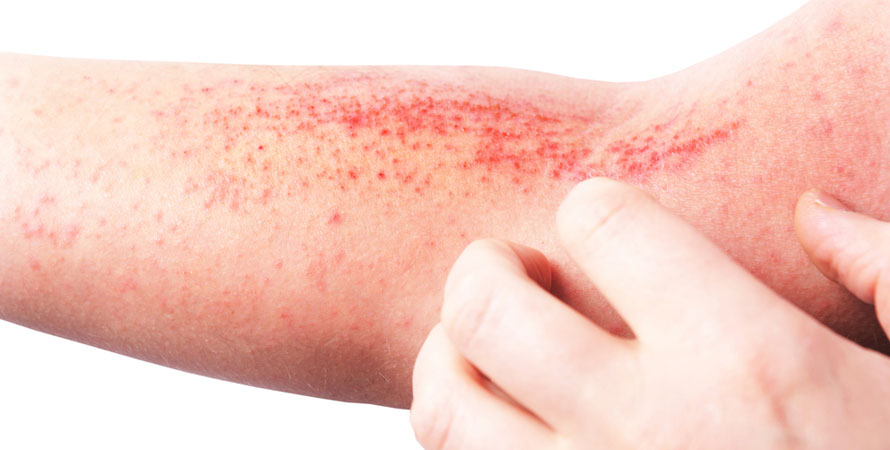
You might have contact dermatitis if you have thick, scaly, and reddened skin that is triggered by an allergic reaction to something you touch.
There are two kinds of it: An immune system reaction to an allergen, such as latex or metal, causes allergic contact dermatitis. A chemical or other substance that irritates your skin is the precursor to irritant contact dermatitis.
Symptoms of eczema
These widespread signs can include dry skin, crusting, inflammation, and itching of the skin. Blisters, seeping clear fluid from flare-ups, and scaly areas are examples of more severe symptoms. People with eczema are more likely to develop skin infections on eczema-affected regions of the skin than people without the condition because eczema damages the skin barrier.
With the right skin care regimen, emollients, and limiting exposure to food allergens that cause eczema flare-ups, some eczema symptoms, such as skin dryness, can be treated. Even individuals with eczema should invest in high-quality moisturizers, lotions, creams, shampoos, and soaps. Additionally, it’s crucial to exercise caution when buying perfumes, dyes, detergents, ointments, and other products because some of them may trigger flare-ups.
Why are psoriasis and eczema frequently confused?
Both psoriasis and eczema are frequent skin disorders that can last a lifetime. Both can result in red, flaky rashes and entail skin irritation. So it is easy to understand why they are frequently confused. But it’s crucial to understand their distinctions.
Despite being two different illnesses, eczema and psoriasis share an important characteristic. The immune system is involved in each of these conditions, but in distinct ways. However, because both conditions can have other origins, neither is considered to be a true autoimmune illness.
What causes psoriasis and eczema?
Eczema and psoriasis triggers might vary from person to person. The following is a list of typical eczema triggers:
- extreme weather or temperature variations
- Stress (physical or mental) (physical or mental)
- sweating and skin rubbing
- Wool or other bothersome fabrics
- Topical allergies, such as some perfumes and preservatives
- prolonged and repeated use of abrasive soaps
Does psoriasis or eczema go away on its own?

Eczema and psoriasis, which are regarded as chronic skin disorders, are now incurable.
However, as previously indicated, by the time they reach adulthood, the vast majority of children with eczema no longer have symptoms. (However, it’s unclear why this occurs.) Thus, there is a possibility that eczema will go away on its own. If it doesn’t, avoiding triggers and keeping skin hydrated can help regulate the condition and prevent severe flare-ups.
Psoriasis, on the other hand, seldom goes away on its own and typically lasts a lifetime.
What quickly heals eczema?
Sadly, there isn’t a quick fix for eczema. In actuality, there is no known treatment for this illness! Fortunately, there are certain therapy choices that can help you control symptoms, and others may be able to quickly reduce symptoms. Consult with a dermatologist or other trained medical practitioner to determine the best course of action for you.
Treatment
Patients with psoriasis have access to a range of therapy choices. These differ depending on the severity, the size of the lesions, and the patient’s preferences. Creams or ointments with corticosteroids, vitamin D or vitamin A derivatives, or coal tar may be beneficial for mild to moderate instances. If the affected area is large and using creams would be impractical or ineffective, light therapy, oral medicines, or injections may be suggested. Otherwise, treatments are still evolving. Many Psoriasis clinical trials are happening around the world to develop better treatments.