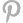What is Small Intestine Bacterial Overgrowth (SIBO) and what is its relationship to Irritable Bowel Syndrome (IBS)?
Small Intestinal Bacteria Overgrowth, or SIBO, is a condition where certain types of bacteria in the small intestine become overgrown for various reasons (https://link.chtbl.com/SIBO). There are three types of SIBO, classified by the kind of gas produced by bacterial fermentation of food in the small intestine and often diagnosed using a breath test. Patients who show high hydrogen gas output on a breath test typically experience more diarrhea than constipation and are considered to have SIBO-D.
Bacteria that produce hydrogen sulfide gas may also cause diarrhea and a new test has just come on the market that includes this gas. One telling symptom of hydrogen sulfide SIBO is a gas that smells like rotten eggs.
Patients with higher levels of methane typically experience more constipation than diarrhea and are considered to have SIBO-C (also known more recently as SIBO-M for methane or IMO – Intestinal Methanogen Overgrowth, as methane is also produced by archaea, which are not bacteria, and may live in the large intestine as well). The third type of SIBO, called mixed-SIBO, refers to patients who experience a mixed pattern of both diarrhea and constipation.
According to naturopath Dr. Nirala Jacobi, an internationally recognized expert in SIBO and a guest on episode 17 of the podcast The Perfect Stool: Understanding and Healing the Gut Microbiome, over 550 million people worldwide (11% of the global population) suffer from SIBO, with 50% struggling with relapsing flares.
Despite these harrowing statistics, according to other sources, including an article published in Therapeutic Advances in Chronic Disease journal from 2013, the true incidence of SIBO is largely unknown because of the difficulty in establishing a baseline standard small intestinal flora and no current testing method meeting ideal standards for validity.
The prevalence of SIBO is particularly difficult to measure because there is an association between SIBO and a number of other disorders, and symptoms often overlap. For instance, the authors cite a prevalence of SIBO in IBS from 30 to 85 percent depending on the source used.
Current diagnosis and testing models

So what does a SIBO diagnosis really mean? How is it confirmed?
A SIBO diagnosis often starts with clinical suspicion, based on a history of risk factors, followed by physical examination by an informed gastroenterologist, naturopath, or functional medicine practitioner.
One test involves a quantitative culture of duodenal aspirates (a sampling of cells from the small intestine) demonstrating greater than 100,000 cfu/ml of fluid. However, this value is not validated, has been contested by systematic review and duodenal aspiration is impractical in the majority of cases.
Another model for SIBO testing, which is now most widely used as an alternative to direct aspiration testing, are breath tests, which are non-invasive and less expensive. The most common breath tests used to diagnose SIBO are hydrogen and methane breath tests, which are based on the principle that carbohydrate fermentation by the gut flora is done primarily by anaerobic bacteria in the colon, which is the only source of hydrogen and methane in the body.
When bacteria from the colon colonize the small intestine, as in SIBO, fermentation of carbohydrate in the small intestine produces a large amount of hydrogen or methane gas.
Hydrogen and methane breath tests are administered following consumption of a low fiber diet for 24 hours and a 12-hour overnight fast. Individuals are asked to exhale into a tube connected to a bag and hydrogen or methane baseline values are obtained.
Afterward, individuals take a carbohydrate substrate orally (most commonly glucose or lactulose, and less commonly xylose), and are asked to exhale every 15 minutes for 3 hours. Like with direct aspiration testing, the criteria for a positive breath test are not well validated.
Dr. Jacobi observes that a lactulose hydrogen breath test and a glucose hydrogen breath test given to the same patient sometimes return conflicting results because of the part of the intestine in which each substrate is digested. For this reason, she will often administer both in the process of confirming a diagnosis.
Despite its continued clinical manifestation, there is no single valid test for SIBO, there is limited agreement on the composition of normal small intestinal flora and there is limited availability of breath testing through traditional doctors and insurance. Consequently, SIBO often goes misdiagnosed or underdiagnosed.
In a pilot interventional study from May 2019, published in Nature Communications researchers found that SIBO, based on a culture analysis of duodenal aspirates, demonstrates that a proliferation of anaerobes (organisms that grow without oxygen), does not correlate with symptoms a patient experiences, and may be a consequence of dietary choices.
In this study, the researchers discovered that patients who switched from a diet high in fiber to a diet low in fiber and high in simple sugar experienced an increase in functional gastrointestinal disorder (FGID)-related symptoms.
The study made two critical observations about the clinical definition of SIBO and its manifestations. First, the study found that SIBO does not correlate with dysbiosis in the small intestine (or an abnormal composition of gut microbes).
Researchers compared the microbial composition of symptomatic patients with and without SIBO and found that some symptomatic patients diagnosed with SIBO actually have an overabundance of bacteria normally found in healthy microbial communities; meanwhile, others, who do not have SIBO, actually have dysbiosis.
In addition to disassociating SIBO and microbial dysbiosis in the small intestine, the study untangled another critical assumption about SIBO, finding that a subset of healthy individuals eating high-fiber diets have SIBO.
The lack of a correlation between SIBO and dysbiosis, and the incidence of SIBO in healthy individuals, raised the question for the researchers of whether SIBO is a primary driver of symptoms of FGIDs, like IBS, or if it indicates simply an environmental influence (i.e., if SIBO appears as the result of dietary factors).
SIFO (Small Intestine Fungal Overgrowth) and its relationship to SIBO
Candida is an important yeast that is present in all healthy people. When an individual has taken a lot of medications, especially antibiotics that kill natural bacteria in the body that keep the growth of Candida in check, Candida can overgrown.
Overgrowth of Candida, also known as Small Intestine Fungal Overgrowth (SIFO), has a higher incidence in individuals who have diets that are high in refined carbohydrates, like sugars and simple starches.
Refined carbohydrates feed Candida and encourage its growth. Roughly 25-30 percent of people who test positive for SIBO also have SIFO. If a person tests positive for SIBO and is experiencing symptoms like sugar cravings, brain fog and rashes, a SIFO diagnosis may be indicated.
However, SIFO is known by clinicians as the “Great Masquerader” for a reason: it often goes undetected on stool tests but can be most accurately diagnosed using an Organic Acids Test. Though herbal treatment for SIFO and SIBO may be similar, halting the growth of Candida in the small intestine takes longer than bacteria, so identifying a SIFO diagnosis is important for determining the length of a treatment plan.
Treatment
Antibiotics are often recommended for SIBO, in particular, Rifaximin, which only kills bacteria in the gastrointestinal tract. The potential drawbacks of this approach are the cost (Rifaximin costs almost $2000 if not covered by insurance), an incidence or worsening of SIFO, stressing of the gut lining, or a potential long-term relapse.
As a result, many gut health experts prefer a longer course of herbal treatments and creating a gut environment that favors the growth of healthy microbes. Many herbal nutraceutical products that address both bacterial and fungal overgrowths at the same time are effective treatments for SIBO.
Because the SIBO diagnosis remains contested, with recent research calling into question the relationship between SIBO and intestinal dysbiosis, treatment to alleviate GI symptoms according to Lucy Mailing, PhD, shouldn’t focus on killing overgrown bacteria. She cites multiple factors that can reduce butyrate in the lining of the small intestine, causing oxygen to leak into the gut, which causes or exacerbates dysbiosis.
These include gut infections, antibiotics, a low-fiber diet and stress. Therefore, changing your diet to include more fiber, avoiding antibiotics, addressing SIFO and managing stress are keys to supporting a healthy gut metabolism. Butyrate supplementation and more advanced interventions may be recommended by your gut health practitioner.
Along with prescription and non-prescription treatments, a low FODMAP (fermentable oligosaccharides, disaccharides, monosaccharides and polyols) diet is often recommended for SIBO. If that’s doesn’t alleviate symptoms, the SIBO Bi-phasic Diet developed by Dr. Jacobi is a more restrictive protocol, although both are meant for short-term use only in order to prevent the extinction of healthy gut microbes.
Discovery of the Autoimmune Nature of SIBO
The recent discovery of antibodies that attack the villi in the small intestine, called anti-CdtB and anti-vinculin antibodies, by Marc Pimintel, MD, points to an autoimmune cause for some portion of SIBO patients.
This usually follows an episode of food poisoning, which triggers an autoimmune process in the body, resulting in impaired motility in the small intestine. The ibs-smart™ test, developed by Dr. Pimintel can determine whether SIBO is autoimmune in nature and if so, a prokinetic drug (a small intestine motility agent) and a lower carbohydrate diet may be recommended in the long term following treatment.
The Connection Between SIBO and Autoimmune Disease
The job of the small intestine is to absorb nutrients while filtering out bacteria, toxins and wastes. Tight junctions, where the membranes of two adjacent intestinal cells join together to form a barrier, are responsible for filtration functions.
Faulty tight junctions can lead to increased permeability in the intestines, or leaky gut, characterized by the escape of partially digested proteins and parts of bacterial bodies that enter the bloodstream and stimulate the immune system.
Dr. Alessio Fasano, a pediatric gastroenterologist, well-known researcher in this field and founder of the University of Maryland Center for Celiac Research, cites three root causes common to all autoimmunity. These factors are: antigen exposure, genetic susceptibility and increased intestinal permeability.
Because intestinal permeability is a typical byproduct of SIBO, it is often found to be the underlying cause of many autoimmune conditions, such as Irritable Bowel Disease (Crohn’s and Colitis), Scleroderma, Celiac Disease and Hashimoto’s Thyroiditis. Therefore, it’s important to address SIBO, SIFO or gut dysbiosis for the prevention and treatment of autoimmune disease.
Conferring a SIBO diagnosis is difficult, given that there is no single valid test for SIBO, there is limited agreement on the composition of normal small intestinal flora, and there is limited availability of breath testing through traditional doctors and insurance.
As a result, SIBO often goes misdiagnosed or underdiagnosed. Nevertheless, clinicians continue to observe health challenges associated with bacterial (as well as fungal) overgrowth in the small intestine. Dr. Marc Pimintel’s recent discovery of antibodies that attack the villi in the small intestine points to an autoimmune cause for some portion of SIBO patients.
The small intestine has the important and complex job of allowing nutrients inside the body while keeping bacteria, toxins and wastes out. Tight junctions, where the membranes of two adjacent intestinal cells join together to form a barrier, are responsible for filtration functions.
Incompetent tight junctions can lead to a higher likelihood of intestinal permeability, or leaky gut.