Many issues and conditions can impact the joints and bones, ranging from mild to severe, and may significantly decrease your quality of life. For example, there are numerous types of arthritis, some of which can lead to bone-related changes such as subchondral sclerosis. Keep reading to learn about the symptoms, causes, and treatment of this problem.
Subchondral Sclerosis: What Does it Mean?
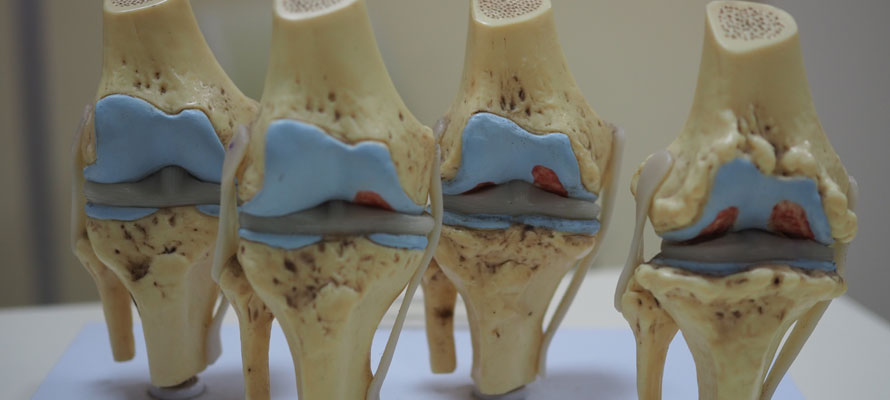
Subchondral sclerosis, or marginal sclerosis, is a thickening of the bone under the joint cartilage. In most cases, this condition affects the hip, knee, spine, sacroiliac joint, and foot. It causes the region below the cartilage layer to fill with collagen, making the bone denser than healthy bones.
The bone impacted in marginal sclerosis is the subchondral bone beneath the cartilage. The name derives from the term chondro, meaning cartilage, and the prefix sub, meaning below. This particular bone functions as a shock absorber in weight-bearing joints.
It is important to note that marginal sclerosis isn’t necessarily a diagnosis in itself, but rather a radiological symptom that occurs due to another condition.
What Causes Subchondral Sclerosis?
Under normal circumstances, the body repairs damaged bone tissue regularly, particularly around your joints. However, in some cases, the tissue becomes dense and has higher collagen levels than normal bone.
You may develop sclerosis spine or the same issue in other joints, and the reasons are not completely clear.
However, the most common potential causes and risk factors include:
- Osteoarthritis (OA): This is the most common cause of subchondral sclerosis. Since OA is a degenerative joint disease, the breakdown of cartilage can cause changes in the underlying bone, leading to this issue. However, not every patient with OA will develop the condition.
- Injury or Trauma: Repeated trauma, injuries, and fractures could lead to changes in the subchondral bone, including sclerosis. This occurs because the body attempts to repair the damaged area by increasing bone density.
- Joint Instability: Instability may lead to abnormal joint loading, meaning the force required for movement. As a result, this may trigger changes in the bone that can lead to the development of subchondral sclerosis.
- Rheumatoid Arthritis (RA): Although sclerosis occurs most commonly with OA, people with RA can develop it too. Since RA is an autoimmune disease, the immune system could start attacking healthy joints, cartilage, and subchondral bones.
- Genetics: Some people have a genetic predisposition to developing sclerosis spine or problems with the subchondral bones. Research [1] indicates that malformations in joint structures caused by genetic mutations could lead to abnormal subchondral bones and contribute to the development of OA. A family history of OA and bone sclerosis may increase this risk.
Overweight or Obesity: Carrying excess weight can put stress on the joints, paving the way to developing OA and symptoms such as bone spurs.
- Age: This is a significant risk factor in developing OA and bone spurs. Over the years, the joints experience considerable wear and tear, and the subchondral bones may also change with age and possibly lead to sclerosis.
- Gender: Women are more susceptible to OA, especially after menopause, due to declining estrogen levels and weight gain that can occur during this time.
What Are the Symptoms of Subchondral Sclerosis?
The symptoms of subchondral sclerosis [2] are similar to osteoarthritis and include:
- Pain and tenderness in the affected areas (usually the hips, knees, spine, and hands)
- Pain that worsens during or after weight-bearing activities and at night
- Stiffness in the affected joints
- Limited flexibility and range of motion
- A grating sensation in the affected joints
- Bone spurs or hard lumps surrounding the affected joints
- Joint swelling
When Does Subchondral Sclerosis Begin?
Subchondral sclerosis that occurs due to OA usually happens in the later stages of the disease. However, this transformation in the bone can also develop before OA damages the cartilage of the affected joint.
Osteoarthritis wears down the cartilage and the subchondral bone beneath it. When that happens, the body attempts to repair the damaged bone, eventually causing it to thicken. The exact timing of the condition varies for different individuals, and it may not occur uniformly across all affected joints. If you have concerns about your joint health and the management of OA, schedule an appointment with your doctor.
The Formation of Subchondral Bone Cysts
In some cases of osteoarthritis, a subchondral cyst may develop, also known as a subchondral lesion or geode. Many people with OA are unaware that they have a cyst unless a doctor spots it in an X-ray during the patient’s follow-up.
On an X-ray, a subchondral cyst appears as a tiny fluid-filled sac or multiple sacs below the surface of the affected cartilage. Despite the name, these are technically not cysts [3] by definition, as they don’t feature an enclosed layer of cells.
Over time, the subchondral cyst hardens into the bone, and the fluid dissipates. Although subchondral cysts may cooccur with OA, not every person with the condition develops them. A study of 806 subjects with painful knee arthritis published in the Open Orthopaedics Journal [4] examined whether cysts are common in this population.
The results indicated that 30.6% of subjects with OA had a subchondral cyst, and the researchers concluded that they were not a cardinal radiological feature of OA. This means most people with OA won’t develop cysts, but it’s still important to attend follow-up appointments regularly.
Although OA is the most common cause of subchondral cysts, it may also occur due to rheumatoid arthritis, injuries, and other factors we discussed.

How is Subchondral Sclerosis Diagnosed?
If you have osteoarthritis, your doctor will take periodic X-rays or order an MRI of the affected area during follow-ups. Imaging tests provide detailed insight into the progression of the disease so the physician can adjust treatment if necessary.
A region of increased density under the cartilage on an X-ray indicates subchondral sclerosis, and it appears as an abnormally white area along the joint line.
How is Subchondral Sclerosis Treated?
There is no one specific treatment for marginal sclerosis, but there are several approaches to managing OA and related symptoms such as bone spurs. These are the most significant methods:
- Physical Therapy: This method focuses on strengthening the muscles surrounding the joints to alleviate strain. A physical therapist tailors a customized exercise plan to address each patient’s needs. Exercise can reduce the discomfort caused by sclerosis spine or bone changes in other body parts, and in addition, low-impact physical activity increases stability, flexibility, and range of motion.
- Weight Loss: Losing excess weight can decrease the stress on weight-bearing joints and alleviate pain. To slim down, combine a healthy diet with regular physical activity. In addition, consider adding Flexoplex joint health supplement to your daily routine to support joint function. Regular intake of Flexoplex can reduce joint pain and inflammation, improve flexibility and mobility, and repair damaged tissue.
- Injections: If your pain is severe, the doctor may prescribe corticosteroid or hyaluronic acid injections directly into the affected joint. These injections can provide relief and reduce discomfort.
- Surgery: The most common surgeries are hip and knee replacements, but this option is only recommended when other approaches fail.
FAQs
Can subchondral sclerosis be cured?
There is no cure for subchondral sclerosis, but it is possible to slow down the progression of OA and relieve the pain and other symptoms by adhering to doctor-recommended treatments and modifying your lifestyle. Follow a healthy diet and engage in low-impact physical activity to improve joint health.
When does subchondral sclerosis occur?
Subchondral sclerosis occurs in the later stages of OA and leads to cartilage degeneration. As a result, you may experience symptoms such as pain, stiffness, and poor mobility. Having this condition doesn’t indicate that the arthritis is progressing, it implies that there are changes in the bones.
While they tend to occur later, changes in the subchondral bone [5] may also appear in early OA and reduce the thickness of the subchondral plate.
Outlook
Subchondral sclerosis occurs when the bones become too dense due to underlying causes like arthritis or injury. There is no specific treatment for this issue, but managing it is part of arthritis treatment.
Keep in mind that most people with OA and rheumatoid arthritis don’t develop marginal sclerosis. If you have this issue, see your doctor regularly, and don’t skip follow-ups. You can help prevent the problem from developing by making lifestyle modifications and taking natural supplements to keep your joints healthy.