Stress is often thought of as a mental or emotional burden, but its effects can reach far beyond the mind. Many people experiencing long periods of stress also report physical symptoms, including unexplained aches and stiffness. This raises an important question: can stress cause joint pain? While joint discomfort is commonly linked to aging, injury, or arthritis, stress may play a hidden role in triggering or worsening these symptoms.
When the body is under stress, it releases hormones like cortisol and adrenaline that can influence inflammation, muscle tension, and pain perception. Over time, chronic stress may contribute to increased sensitivity in the joints, reduced mobility, and flare-ups of existing joint conditions. Understanding this connection is essential for anyone dealing with persistent joint pain without a clear physical cause.
In this article, we’ll explore how stress affects the body, the link between stress and joint pain, common warning signs, and practical ways to manage stress to support better joint health.
How stress affects the body: the biological picture
To evaluate can stress cause joint pain, it’s important to review what stress does inside the body. Acute stress activates the sympathetic nervous system and the hypothalamic–pituitary–adrenal (HPA) axis, elevating adrenaline and cortisol. Over time, repeated activation of these systems can alter immune responses, promote chronic low-grade inflammation, and change how the central nervous system processes pain.
- Adrenaline and sympathetic activation: Short-term increases in heart rate and muscle tension can protect you in danger, but recurrent sympathetic activation leads to persistent muscle tightness and wear on joints.
- HPA axis and cortisol: Cortisol helps regulate inflammation, but dysregulated cortisol patterns—whether elevated baseline cortisol or flattened diurnal rhythm—can disturb immune balance. That’s why cortisol and inflammation are central to the question can stress cause joint pain.
- Immune signaling: Psychological stress can raise circulating pro-inflammatory cytokines such as IL-6 and TNF-alpha. These mediators affect joint linings and pain receptors and are one pathway linking stress and joint pain.
These mechanisms answer part of the question can stress cause joint pain: by increasing inflammation and altering pain processing, stress can exacerbate or unmask joint symptoms. But the relationship is complicated by behavior: stress also changes sleep, activity, and diet—each a factor in joint health.
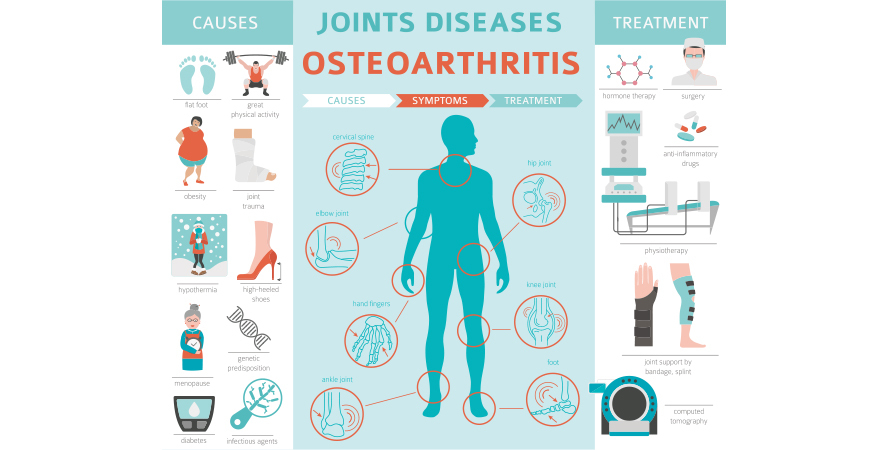
Key mechanisms linking stress and joint pain
Multiple overlapping pathways explain why many people wonder does anxiety cause joint pain or can emotional stress cause joint pain. Below are the major mechanisms that researchers and clinicians cite when discussing whether can stress cause joint pain.
- Inflammation and immune activation
One of the clearest biological links in the can stress cause joint pain conversation is inflammation. Chronic psychological stress is associated with higher levels of pro-inflammatory cytokines. These pro-inflammatory signals increase pain sensitivity and can exacerbate conditions like osteoarthritis and rheumatoid arthritis. When researchers look for objective changes that answer can stress cause joint pain, elevations in IL-6 and TNF-alpha are commonly cited.
Acute stress can transiently suppress some immune functions, but chronic stress tends to increase inflammatory tone. Because joints are sensitive to inflammatory mediators, stress and joint pain are often linked through this inflammatory pathway. The phrase cortisol and inflammation belongs at the center of this explanation: stress changes cortisol patterns, and altered cortisol and inflammation together influence joint health and pain perception.
- Muscle tension and mechanical load
Stress tightens muscles. People who experience stress, anxiety, or emotional upheaval often hold tension in the neck, shoulders, lower back, and around joints. Over time this tension increases mechanical load on joints and can cause or worsen pain. That leads many to ask does anxiety cause joint pain when the primary issue seems to be muscle tightness from emotional stress.
So while structural joint damage is not directly caused by stress in most cases, the additional strain from chronically tense muscles can accelerate wear and create localized pain that patients report as joint pain. This is why clinicians include physical therapy and relaxation techniques when treating patients who ask can stress cause joint pain.
- Central sensitization and pain amplification
Another important mechanism answering can stress cause joint pain is central sensitization. Prolonged stress changes how the nervous system interprets signals, lowering thresholds for pain and amplifying pain signals even when peripheral joint stress is small. Central sensitization helps explain why two people with similar joint degeneration may report very different pain experiences—one may ask can stress cause joint pain because their pain increases during stressful periods.
Stress and joint pain interact within the brain’s pain networks, and does anxiety cause joint pain in part because anxiety primes those networks to respond more strongly. Treatments that target central sensitization—CBT, graded exposure, and mindfulness—often help reduce pain intensity even without changing the underlying joint pathology.
- Behavioral and lifestyle pathways
Behavior is an essential component of why people wonder can emotional stress cause joint pain. Stress frequently disrupts sleep, reduces motivation for exercise, encourages poor dietary choices, and increases alcohol or tobacco use. Each behavior can worsen pain or slow healing: poor sleep increases pain sensitivity, inactivity weakens muscles that stabilize joints, and unhealthy diets can promote systemic inflammation.
In observational studies, stress and joint pain correlate largely because stress disrupts the behaviors that protect joint health. Managing stress can therefore have direct biological effects (less inflammation) and indirect behavioral effects (more exercise, better sleep), both of which reduce joint pain over time.
Common treatments, supplements, and topical options: how they’re made and why people use them
When people search for remedies they often ask can stress cause joint pain and then look for supplements, topical treatments, or quick fixes. Below we summarize common options—how they’re made, their ingredients, the rationale for use, and the evidence base—so you can evaluate claims critically.
- Glucosamine and chondroitin
How they’re made: Glucosamine sulfate is commonly produced from shellfish shells or via synthetic processes, while chondroitin sulfate is extracted from animal cartilage (bovine, porcine, or shark). Vegan glucosamine can be made through fermentation, and these ingredients are commonly combined in joint-support products such as the Flexoplex Joint supplement.
Ingredients and rationale: These molecules are components of cartilage; people take them to support joint tissue or reduce symptoms of osteoarthritis. When patients ask can stress cause joint pain and explore supplements for relief, glucosamine and chondroitin are often among the first options considered.
Evidence: Clinical trials show mixed results. Some people report modest improvement in pain and function, while others see no meaningful benefit. Results can vary based on formulation quality and individual response.
- Omega-3 fish oil
How it’s made: Extracted from fatty fish and purified to concentrate EPA and DHA; many products are molecularly distilled to remove contaminants.
Ingredients and rationale: EPA and DHA have anti-inflammatory properties. For inflammatory arthritis, omega-3s can reduce systemic inflammation and modestly improve symptoms, reinforcing why discussions of can stress cause joint pain often include omega-3s as a supportive therapy.
Evidence: Trials demonstrate modest benefit, particularly in inflammatory conditions like rheumatoid arthritis. Dose and purity matter.

- Turmeric/curcumin
How it’s made: Curcumin is a concentrated extract from turmeric root, often combined with piperine or special delivery systems to enhance absorption.
Ingredients and rationale: Curcumin has anti-inflammatory effects in lab studies and may reduce pain in osteoarthritis or inflammatory conditions.
Evidence: Some randomized trials show small to moderate benefits, but formulations and dosing vary widely. Because curcumin can interact with blood thinners, people considering supplements should consult clinicians—especially when they also wonder does anxiety cause joint pain and plan to self-treat.
- MSM and collagen supplements
How they’re made: MSM is a sulfur compound produced synthetically or derived from natural sources. Collagen supplements come from hydrolyzed bovine, porcine, or marine collagen broken into peptides.
Rationale and evidence: MSM may reduce inflammation; collagen provides amino acids that theoretically support connective tissue. Evidence is preliminary but suggests possible modest symptomatic benefit for some users.
- CBD oil and hemp extracts
How they’re made: CBD is extracted from hemp using CO2 or ethanol extraction and then formulated into oils, capsules, or topicals.
Ingredients and rationale: CBD interacts with the endocannabinoid system and may modulate pain and inflammation. People with chronic pain who ask can stress cause joint pain sometimes try CBD as part of a broader approach to symptom relief.
Evidence and caution: Human trials are limited and mixed. Quality control varies. CBD can interact with medications via CYP450 pathways, so check with a clinician.
- Topical analgesics: menthol, capsaicin, and topical NSAIDs
How they’re made: Formulated as creams, gels, or patches delivering actives locally.
Ingredients and rationale: Menthol produces a cooling sensation, capsaicin depletes substance P to reduce pain signaling, and topical NSAIDs (like diclofenac gel) reduce local inflammation with less systemic exposure. For people asking can stress cause joint pain with localized symptoms, topical treatments can be a low-risk option to try.
Evidence: Topical NSAIDs and capsaicin show effectiveness for certain types of osteoarthritis and localized musculoskeletal pain.
Limitations, risks, and precautions
While it’s tempting to assume can stress cause joint pain and then treat only the stress, important caveats remain.
- Serious causes of joint pain—septic arthritis, crystal arthropathies (gout), fractures, or rapidly progressive inflammatory disease—need urgent evaluation. Don’t assume all joint pain is stress-related.
- Supplements are not tightly regulated. Product quality varies. Look for third-party testing and consult your clinician, especially when considering supplements alongside prescription medications. This is crucial when evaluating whether can emotional stress cause joint pain because some people self-treat rather than seek medical evaluation.
- Drug interactions: glucosamine, omega-3s, curcumin, and CBD can interact with anticoagulants and other drugs. Discuss medication safety with a pharmacist or clinician.
- Allergies and dietary restrictions: glucosamine from shellfish or collagen from animal sources may be problematic for some individuals.
- Oral NSAIDs carry risks with prolonged use—GI bleeding, cardiovascular events, and kidney injury. Topical options may be safer for localized pain.

Practical, evidence-based strategies for people asking can stress cause joint pain
If you suspect stress and joint pain are linked for you, the following approach balances medical evaluation with lifestyle and stress-management strategies:
Get a medical evaluation
See a healthcare provider to rule out urgent or treatable causes of joint pain. If you’re repeatedly asking can stress cause joint pain, make sure structural, infectious, or inflammatory causes are considered and treated appropriately.
Prioritize evidence-based lifestyle measures
- Exercise: Low-impact aerobic activity and targeted strength training reduce joint pain and improve function. Programs like walking, cycling, aquatic therapy, and supervised strength training are beneficial.
- Weight management: Reducing excess weight decreases load on weight-bearing joints and lowers systemic inflammation.
- Sleep: Improve sleep hygiene because poor sleep amplifies pain and reduces stress resilience. Sleep and the question can stress cause joint pain are intimately linked—poor sleep increases pain sensitivity and stress.
Integrate stress-management techniques
If you ask does anxiety cause joint pain or can emotional stress cause joint pain, consider evidence-based stress-reduction strategies:
- Cognitive behavioral therapy (CBT) or pain-focused CBT
- Mindfulness-based stress reduction (MBSR)
- Progressive muscle relaxation and guided imagery
- Biofeedback and paced breathing
These interventions reduce perceived stress, reduce catastrophizing, and often lower pain intensity. They also influence cortisol and inflammation—so learning to manage stress can change physiological drivers of pain.
Use targeted topical treatments for localized pain
Topical NSAIDs, menthol, and capsaicin can reduce localized joint pain with fewer systemic risks than oral medications. For people asking can stress cause joint pain with focal knee or hand pain, topical agents are useful options to try under medical guidance.
Consider supplements thoughtfully
If you decide to try supplements to complement stress reduction and exercise, follow safe practices:
- Consult your clinician or pharmacist before starting supplements—especially if you take anticoagulants or other prescription medications.
- Choose brands with third-party testing (USP, NSF, or ConsumerLab).
- Start one product at a time and give it several weeks to months to assess benefit.
- Keep expectations realistic: supplements may offer modest symptom relief but rarely cure structural joint disease.
When to seek urgent care
While many people ask can stress cause joint pain, some symptoms require urgent attention. Seek immediate care if you have sudden severe joint swelling with fever, rapidly worsening pain, inability to use the limb, or signs of systemic infection. If stress or mood symptoms are overwhelming or suicidal thoughts occur, seek urgent mental health support.
Frequently Asked Questions
Q: Does anxiety cause joint pain directly?
A: Anxiety can contribute to joint pain through muscle tension, altered pain perception, and stress-induced inflammation. So does anxiety cause joint pain? It often contributes as part of a multi-factorial picture rather than being the lone cause.
Q: Can emotional stress cause joint pain even if scans look normal?
A: Yes. Emotional stress can amplify pain perception through central sensitization and increase inflammatory signaling even when imaging shows minimal structural changes. That is part of why many people ask can emotional stress cause joint pain and find relief from stress-targeted therapies.
Q: What is the role of cortisol and inflammation in joint pain?
A: Cortisol modulates immune responses. Chronic stress alters cortisol patterns, which can promote a pro-inflammatory state. The interplay of cortisol and inflammation is a key biological route by which stress affects joint pain.
Q: Will managing stress cure my joint pain?
A: Managing stress can significantly reduce pain and improve function but rarely cures structural joint disease alone. A combined approach—medical treatment when needed, exercise, weight management, and stress reduction—offers the best outcomes.
Summary and final thoughts
In conclusion, stress is more than just an emotional challenge—it can have real physical effects on the body, including joint discomfort. Chronic stress may contribute to inflammation, muscle tension, and increased pain sensitivity, all of which can aggravate existing joint issues or trigger new symptoms. While stress may not be the sole cause of joint pain, it can play a significant role in making the condition worse or harder to manage.
Recognizing the connection between stress and joint pain is an important step toward relief. Combining stress-management techniques such as regular exercise, mindfulness, adequate sleep, and relaxation practices with proper medical guidance can help support both mental well-being and joint health. By addressing stress alongside physical factors, it becomes easier to reduce discomfort and improve overall quality of life.